Understanding Blood Types
Blood types are a fundamental aspect of human biology, determined by the presence or absence of specific antigens on the surface of red blood cells. The two primary systems used to classify blood types are the ABO and the Rh systems. These systems categorize blood into different types: A, B, AB, and O, with each type further classified based on the presence (+) or absence (-) of the Rh factor, commonly known as the Rhesus factor.
The Significance of Blood Type Compatibility
Blood type compatibility plays a critical role during blood transfusions. When blood is transfused from a donor to a recipient, compatibility between the donor and recipient’s blood types is essential to avoid adverse reactions. The immune system is designed to recognize antigens that are foreign to the body, and this includes blood group antigens. If incompatible blood is introduced into the body, it can lead to serious and potentially life-threatening immune responses. Thus, understanding and knowing your blood type is vital for both donating and receiving blood safely and effectively.
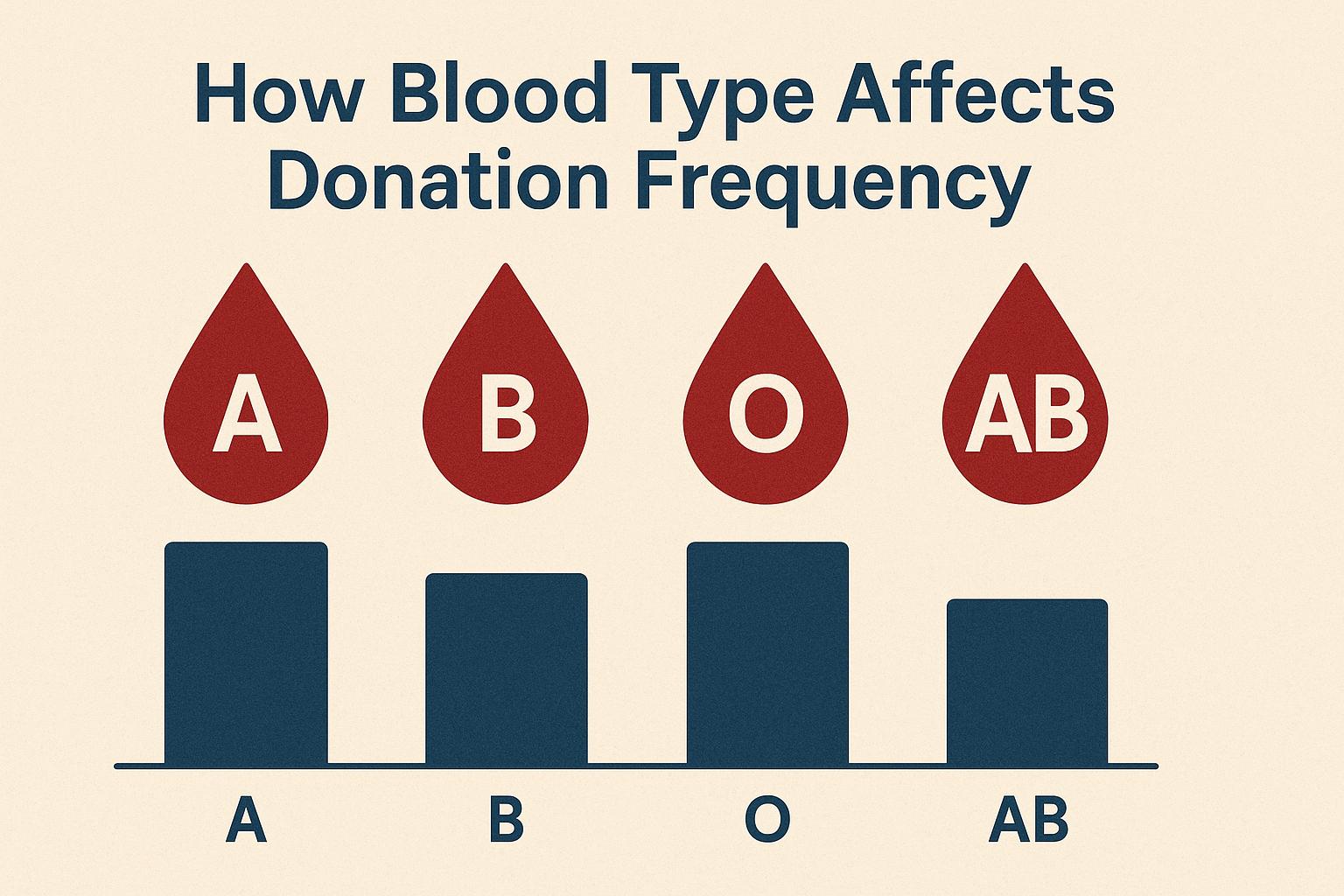
Blood Type and Donation Frequency
The distribution of different blood types varies among populations, and this affects the frequency with which individuals of each type are asked to donate blood. Understanding which blood types are more prevalent can help in organizing effective blood donation campaigns.
Type O blood is one of the most commonly requested blood types. This is because type O blood, particularly O-negative, can be transfused to almost any patient regardless of their blood type. O-negative is often referred to as the universal donor blood type since it lacks the A, B, and Rh antigens that could trigger an immune response in the recipient. Due to its versatility and the high percentage of the population with type O blood, individuals with this blood type are frequently encouraged to donate as their contributions are always in high demand.
Type A blood donors also play a crucial role in maintaining a sufficient blood supply. A-negative blood is less common and, like O-negative, is often in high demand due to its scarcity. A-positive donors are advantageous for their plasma, which can be transfused to any patient with a positive blood type, further proving the importance of these donors in the healthcare system.
Type B is less common in the population compared to types O and A, which makes B-negative the least common type in the ABO blood group system. Given its rarity, donors with B-negative blood are critical in situations where B or AB patients require blood transfusions. Ensuring a stable supply of B-negative blood is essential to meet the needs of those rarer blood type patients.
Type AB blood is the rarest ABO blood type. This rarity also makes AB plasma highly valuable because individuals with type AB blood are universal plasma donors, meaning their plasma can be used for patients of any blood type. Plasma donations from type AB individuals are crucial for maintaining a diverse and adequate blood supply, particularly for patients who require plasma rather than whole blood or red cells.
Encouraging Consistent Donations
Maintaining a stable and secure blood supply demands regular donations from people of all blood types. Blood donation centers frequently highlight and call for donations based on current shortages, with particular focus placed on the blood types most in demand at any time. By being informed about these ongoing needs, donors can actively participate in ensuring that critical blood components are always available for those in need.
Blood donation centers such as The American Red Cross are pivotal in providing real-time updates on blood needs and organizing specific donation campaigns. Active donor awareness and participation mean that people, irrespective of their blood type, can significantly contribute to a comprehensive and life-saving blood supply.
The Role of Public Awareness
Public awareness of the importance of blood donation is vital. While certain blood types may be in higher demand, every donation is valuable and contributes to saving lives. Community engagement and collaboration with medical centers can foster a culture of regular and voluntary donation. The increase in public awareness around the significance of blood donation can lead to a more resilient blood supply, safeguarding access to necessary transfusions for all patients in need.
Furthermore, educational campaigns are crucial in informing the public of the seamless and straightforward nature of donating blood, as well as dispelling any misconceptions or fears about the process. As more individuals become aware of the impact their donations can have, the more robust our communal blood supply will become.
Ensuring that adequate levels of blood are available requires the commitment of regular donors, emergency donors who step up during critical shortages, and new donors appending their contributions to the established pool. By nurturing a well-informed society aware of the needs and processes of blood donation, we can secure this invaluable resource for those whose lives depend on it.
This multifaceted approach to blood donation not only ensures a steady and diverse supply of blood and blood products but also builds a cooperative community health resource that can respond quickly to large-scale emergencies, sudden medical demands, and routine surgeries and procedures.